Nationwide Outcomes of Less Invasive Mitral Surgery versus Conventional Sternotomy: Analysis of the STS Adult Cardiac Surgery Database; A Summary
In the ongoing debate and controversy surrounding less invasive surgery when treating mitral pathology, McGovern Medical School at UTHealth, Cardiothoracic and Vascular Surgery faculty, Tom C. Nguyen MD, and Charles C. Miller PhD, along with research fellow, Alex Nissen MD, are in the initial developmental stages to compare less invasive mitral surgery (LIMS) to conventional sternotomy. In effort to shorten the knowledge gap surrounding short-term outcomes and repair rates of LIMS versus sternotomy, the McGovern team has worked to create the analysis and research study with their cardiothoracic surgery colleagues including: Vinod H. Thourani MD, of Medstar Heart and Vascular Institute at Georgetown University, Y. Joseph Woo MD of Standford University School of Medicine, James S. Gammie MD of University of Maryland School of Medicine, and Gorav Ailawadi MD, with University of Virginia, Charlottesville, VA.
By utilizing the Society of Thoracic Surgeons (STS) Adult Cardiac Surgery Database, as well as national, multicenter data, the research team over the next few months will work towards building, defining, and theorizing their hypothesis:
“We hypothesize that clinically significant differences in rates of valve repair, perioperative morbidity and postoperative outcomes exist when comparing LIMS versus conventional sternotomy.”
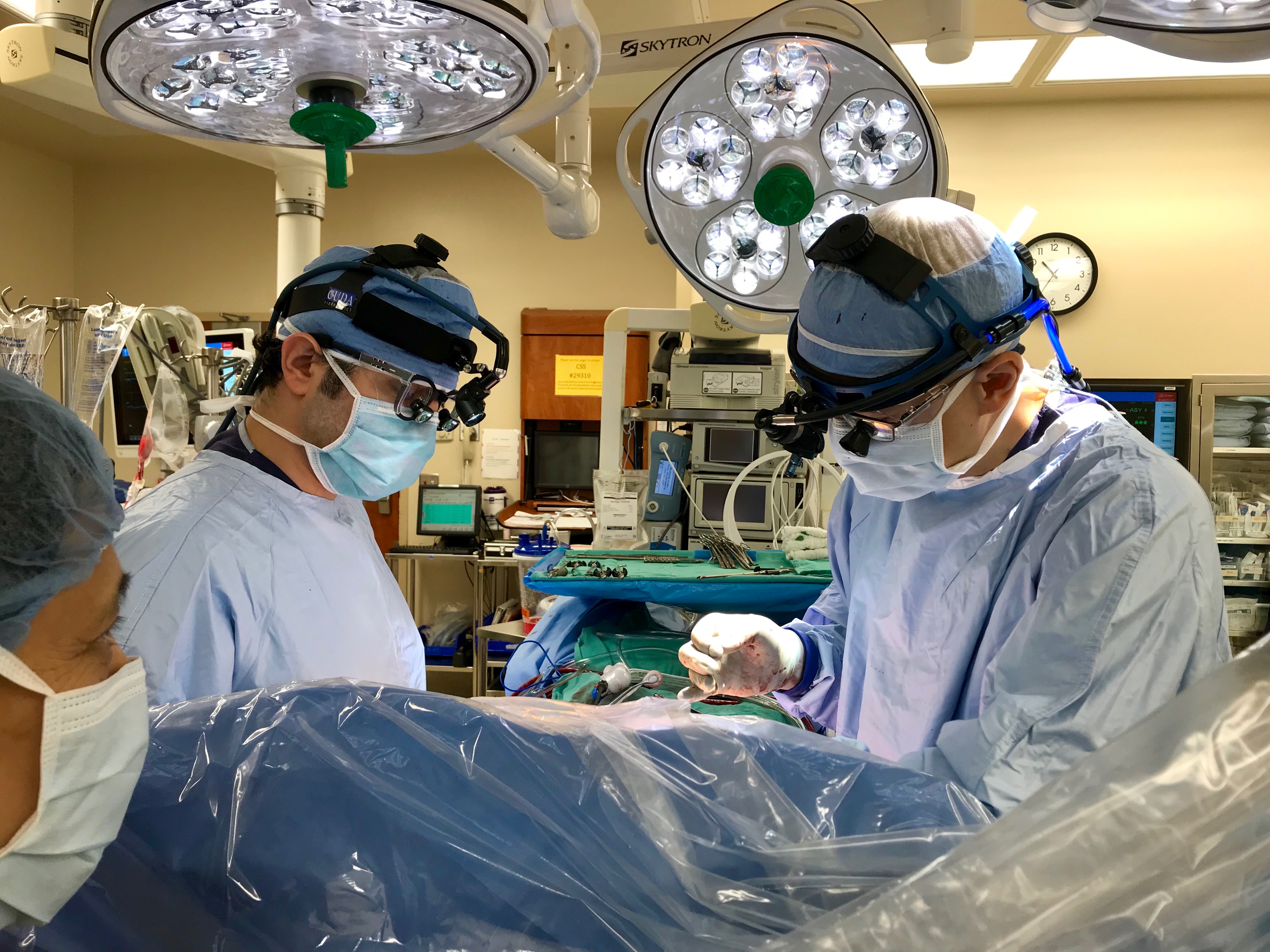
Aortic Surgery Fellow, Kenton Rommens, MD (left) and Associate Professor, Cardiothoracic Surgery, Tom C. Nguyen (right) in a minimally invasive mitral valve procedure.
According to preliminary research conducted, surgical specialists advocating for LIMS suggest that there is a reduction in blood transfusions, atrial fibrillation and length of stay, whereas those in favor of traditional sternotomies argue that LIMS is related to an increased learning curve, extended operative times, and lack the ability to address complex mitral pathology. While previous studies examining these differences have been primarily specific to single-center data sets, Nguyen and his team seek to collect recent and up-to-date data, and combine these sets to compare the information on a broader scale, nearing 90,000 cases. Objectives to be addressed during the study, include:
- Compare perioperative outcomes and short-term mortality between LIMS versus conventional sternotomy.
- Compare repair rates between LIMS versus conventional sternotomy.
- Compare mitral pathologies (e.g. degenerative posterior/anterior/bi-leaflet, functional, mitral annular calcification) and patient risk profile between LIMS versus conventional sternotomy.
- Examine what clinical and/or institutional factors predict the decision to perform LIMS versus conventional sternotomy.
- For all those that get a REPAIR, what % are LIMS v STERN. For all those that get REPAIR, breakdown of surgical/institutional volume. For all those that get REPLACEMENT, breakdown of surgical/institutional.
- Determine the role of surgeon and institutional volume in predicting mitral repairs rates and outcomes in LIMS versus conventional sternotomy.
Tables collecting information to be analyzed include: Preoperative Patient Characteristics, Intraoperative Variables, Mitral Valve Repair or Replacement Details, and Postoperative Outcomes. By evaluating a broader sample size, and modernizing outdated LIMS treatment data, the team hopes to solidify the validity of LIMS, and to clarify the role LIMS has when treating mitral pathology.
-Caliann Ferguson, Marketing Coordinator, Department of Cardiothoracic and Vascular Surgery at McGovern Medical School, UTHealth
This has been a summary of “Nationwide Outcomes of Less Invasive Mitral Surgery versus Conventional Sternotomy: Analysis of the Society of Thoracic Surgeons Adult Cardiac Surgery Database”. This paper has not yet been published.