Trauma Team Activation Policy
Original Date: 06/2016 | Last Review Date: 11/2025
Purpose: To provide consistent guidance for the identification of patients who require a trauma team activation.
Injured patients will be categorized and given a code level based on criteria in this guideline.
Applies to all patients with trauma mechanism of injury within 48 hours of presentation.
A. The trauma team will be group paged using Trauma Page software from a PC terminal in one of four locations: Emergency Center Triage, Trauma, Life Flight Dispatch, and EMS triage desk. The following information is required to determine the appropriate level of response.
- Patient’s approximate age, gender, ETA to Memorial Hermann Hospital, GCS, systolic blood pressure, respiratory rate, pulse and mechanism of injury
- Anatomical findings
- Mechanism of injury
The Trauma Page software program will determine the appropriate level of response and automatically page the appropriate team members.
In the event of a rapid decline in the patient status and emergent activation of the trauma team is required, upgrade the patient and use Trauma Page to page out a Level 1.
In the event of a malfunction of the Trauma Page software or associated computer hardware, the support center will be notified of the issue. The following process will be used to notify the trauma team of patient’s arrival:
- The Life Flight communications office will notify the emergency center charge nurse and identify to them that the Trauma Page system is not working and relay information above on the incoming trauma patient including the code level.
- The emergency center charge nurse will notify the trauma EC attending and the Trauma Chief. The Trauma Chief will notify the Trauma Attending.
B. Tiered response for Adults – the following criteria will be used to determine the level of activation required for patients care aged 16 years and above.
| Response Tier Level | Criteria | Personnel |
|---|---|---|
| Level 1 (Most Severe injuries) |
|
Response Team Trauma Attending Trauma PGY 4-5 Trauma PGY 2 Trauma PGY 1 EM Attending EM PGY 2/3 EM PGY 1 EC RN x2 Radiology Resident Radiology Tech Respiratory Tech Trauma Medical Students Also Notified |
| Level 2 (Moderate Injuries) |
None of the above findings and any of the following:
|
Response Team EM Attending EM PGY 2/3 EM PGY 1 EC RN x2 Radiology Tech Also Notified |
The trauma service may be consulted at the discretion of the ED attending at any time. Please contact the trauma faculty on call if the ED is experiencing undue delay in trauma consultation. The telecom secretary in the ED has a current list of all trauma faculty mobile phone numbers.
Level 1 patients may be downgraded after a mutual agreement between ED faculty and Trauma faculty/fellow following primary and secondary survey, FAST, and screening CXR/PXR as indicated.
Trauma Team Roles and Response for Level 1 activations
General Pre-arrival Preparation
- All trauma team members who anticipate direct patient contact
- Assume a protective gown, gloves, shoe coverings, protective mask, goggles or glasses, and head cover
- Assemble in the assigned resuscitation room and sign in on time out board. Assume assigned position and state their name and role to the nurse recorder
- Physician Staff
- Trauma team leader will assign specific roles and tasks to available physicians and medical students
- Nursing Staff
- Bring in trauma cart
- Ensure Belmont infuser is in room, ready and accessible
- Prepare specimen collecting supplies
- Trauma Technician
- Responds to blood bank on patients arriving with blood infusing prior to arrival and brings the initial cooler of products
- Radiology Staff
- Respond to Trauma Team Code
- Ensures requested images are ordered in the computer
- Completes requested images
- Provides final interpretation of screening CT scans (head, C- spine, CAP) within 12 hours
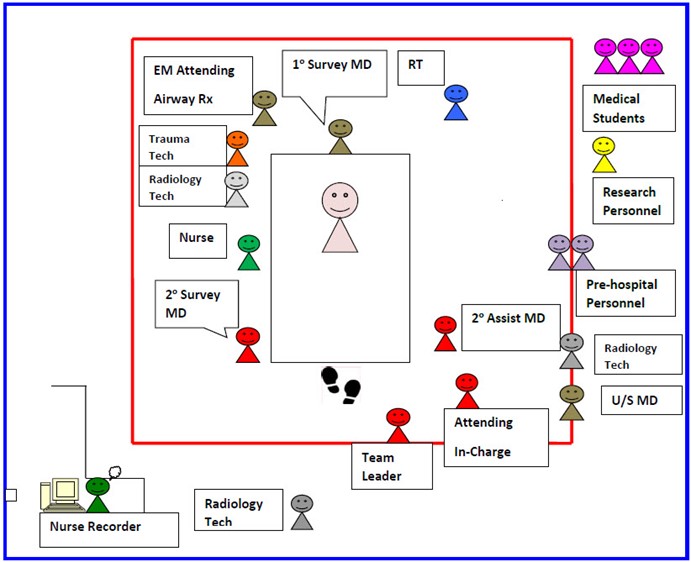
Arrival Management (See diagram for positions in trauma room)
- Pre-hospital Personnel
- Gives report while patient is moved to the trauma stretcher
- EMS and Hospital staff move patient to trauma stretcher
- Attending in Charge/Team leader (Trauma and/or EM physician if trauma not present)
- Utilize ATLS guidelines to supervise primary survey, secondary survey and resuscitative measures as deemed necessary
- Assume responsibility for the evaluation and management of the injured patient until transfer of care to the appropriate service attending or until discharge of the patient from the emergency center
- Maintain open and active communication with the trauma team leader
- Authorize consultations to specialty services
- Review and supervise the documentation of evaluation and management of care
- Facilitate the work up by reviewing radiology films as they become available
- Limits the number of people at the bedside to only those who are essential for initial evaluation, management and direct authorized observers to remain outside the designated trauma evaluation space
- Communicate directly to team
- Primary Survey (EC MD head of bed)
- Perform a rapid primary survey
- Identify the need for difficult airway cart
- Perform procedures as directed by the team leader
- Secondary Survey (Trauma Team MD Member left side of bed- facing patient)
- Assist in exposing the patient
- Perform secondary survey
- Perform assigned procedures and task
- Ensures adequate access of 2 large bore IV’s, if unavailable inserts cordis and obtains blood sample
- Supervise medical student participation in procedures at the discretion of the team leader
- Secondary Assist (Trauma Team MD Member right side of bed facing patient)
- Assist with exposing the patient
- Do task as directed by team leader
- RN (Recorder)
- Documents care on trauma template
- Document arrival times & names of trauma team
- Initiates and signs the level 1 MPP order set
- Receive and document report from pre-hospital personnel or triage RN including mechanism of injury, GCS, assessment, physical findings, interventions, medications, type and volume given
- Document all findings during primary and secondary assessment
- Document fluids, blood and medications as announced
- Ensure patient is monitored during all diagnostic tests
- Document interventions as they are performed
- Complete patient documentation
- Assure ICU, IR, or floor is notified with patient report and estimated time of arrival
- Document vital signs and neurologic status as clinically indicated and with any significant changes
- RN (Circulating RN)
- Obtains initial B/P manually and ensures collection of vital signs including a temperature in the initial set
- Obtain large bore peripheral IV access and blood samples
- Ensure patient remains covered with warm blankets after secondary survey and resuscitative measures are completed
- Ensures recorder RN aware of all interventions and procedures performed
- Administer medications ordered by the trauma team leader
- Announce amount of crystalloid and blood products infused
- Ensures allergy and blood band are on the patient
- Prepares patient for immediate critical transport
- Trauma Technician
- Announces the initial cooler of products arrival
- Ensure that previous patient is discharged from monitor
- Ensure the new patient is admitted to monitor and sets B/P to repeat Q 3 minutes. Also calls out first set of electronic V/S including temperature to recording nurse.
- Place monitor leads on patient
- Ensure patient remains covered with warm blankets after secondary survey and resuscitation measures
- Deliver blood sample to lab and to blood bank and announces “Trauma team activation level 1”
- Patient Access
- Register patient
- Confirms Life Flight ID number
- Collect, label, and secure patient valuables
- Documents patients’ valuables on inventory list and places a copy of the inventory list with patient chart
- Charge RN
- Ensures and coordinates availability of beds
- Assist to facilitate a smooth and prompt transfer out of EC
- When hospital beds are not promptly available, provide ongoing communication to the trauma team leader, attending, and operations administrator regarding problems and/or progress in obtaining a bed
- Radiology Tech
- Obtain images requested by trauma team leader
- Assist the team leader or assigned member in arranging for all subsequent radiological studies
- Radiology Resident/ Fellow/ Attending
- Be available to evaluate x-rays and CT scans as soon as they are processed and provide a prompt report in PACS
- Notify trauma team leader of any changes between the preliminary and the final report
- Respiratory Therapy
- Ensure ETT is secure after handoff of airway management (ETT)
- Adjust as instructed after imaging
- Attach, monitor and document end tidal CO2 monitor
- Manage ventilator and hand bagging as required
- Ultrasound Resident
- Perform F.A.S.T ultrasound and announces findings
Trauma Team Roles