Balloon Eustachian Tuboplasty for Chronic Eustachian Tube Dysfunction
 Two weeks after having balloon eustachian tuboplasty, Robin Goebel was on a flight to South America, where she hiked at high altitudes, visiting Machu Picchu at 7,970 feet and Cusco at 11,152 feet, and took 13 different flights to places ranging from Ecuador to the Galapagos Islands. Prior to the procedure, she was plagued by persistent ear pressure and severe pain when she traveled by air.
Two weeks after having balloon eustachian tuboplasty, Robin Goebel was on a flight to South America, where she hiked at high altitudes, visiting Machu Picchu at 7,970 feet and Cusco at 11,152 feet, and took 13 different flights to places ranging from Ecuador to the Galapagos Islands. Prior to the procedure, she was plagued by persistent ear pressure and severe pain when she traveled by air.
Goebel found Martin J. Citardi, MD, when her ENT referred her to Houston after five sinus surgeries in Beaumont, Texas, a 90 minute drive from Houston. Five years ago Dr. Citardi performed a revision sinus surgery to treat “pockets of smoldering infection with significant scar tissue.” She did well after the procedure.
Now 52, Goebel has suffered from chronic rhinosinusitis and severe allergies since her teenage years in Florida and during later life in Texas. “When Robin developed eustachian tube dysfunction, we knew we could help her,” says Dr. Citardi, professor and chair of the Department of Otorhinolaryngology-Head and Neck Surgery at McGovern Medical School at UTHealth. “Eustachian tube dysfunction’s exact trigger is unknown, but it is associated with inflammation in the nasopharynx, something we expect with chronic rhinosinusitis.”
In an article published in the International Forum of Allergy & Rhinology in 2017, Dr. Citardi and his colleagues noted that ear symptoms are common among patients who present at a rhinology clinic. In a prospective study of 492 patients, 43.3 percent reported symptoms consistent with a formal diagnosis of eustachian tube dysfunction.
“Confirming the diagnosis can be tricky,” says Dr. Citardi, who is chief of otorhinolaryngology at Memorial Hermann-Texas Medical Center. “We need a history supportive of the diagnosis and an abnormal tympanogram suggesting fluid in the middle ear. If we have chronicity of symptoms for at least three or four months, we consider surgery.”
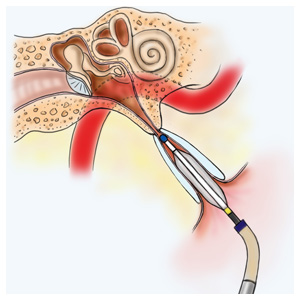
The traditional surgery involves placing a tympanostomy tube in the patient’s tympanic membrane; the new procedure uses the Acclarent AERA® Eustachian Tube Balloon Dilation System, in which a balloon catheter is placed into the eustachian tube through its opening in the nasopharynx under direct visualization with a nasal telescope. Once placement of the balloon ins confirmed, it is inflated with saline for 2 minutes. The saline is then removed to deflate the balloon, and the catheter device is removed.
“Device placement is important,” Dr. Citardi observes. “Trauma can cause damage to the tissues of the nose. We also do a CT before the procedure to avoid carotid artery injury.”
Goebel describes Dr. Citardi as “a godsend. “ She adds, “My seasonal symptoms are 100 times better, and since I had the revision sinus surgery, this is the longest I’ve gone without another sinus surgery,” she says. “At one point I was in the OR every three or four months. I was so sick that it affected my work, my home life and my family. Then I developed the problem with my ears and couldn’t travel without intense pain. I’m happy to be able to resume a normal life.”
Reference
Marino MJ, Ling LC, Yao WC, Luong A, Citardi MJ. Eustachian tube dysfunction in patients treated in a tertiary rhinology clinic. Int Forum Allergy Rhinol. 2017;7:1135-39.
Schedule an Appointment
Call Us
To schedule an appointment over the phone, give our office a call at (713)-486-5019.
Online Appointment Requests
Patients may submit their appointment requests through our online Appointment Request Form.
Both current and new patients can request appointments through MyUTHealth, our patient portal.