Surgical and Clinical Skills Center
McGovern Medical School Surgical & Clinical Skills Center (SCSC) was completed in 2005. The Center provides hands-on education, training, and quality improvement initiatives to many individuals at differing levels of training. As the name implies, the center brings a unique learning location focusing on both the clinical training and the “hands-on” aspect of healthcare. This combination of both areas under one educational facility provides the most sophisticated learning environment for the healthcare community.
The SCSC has a very robust standardized patient (SP) program. The standardized patient program provides teaching and assessment learning opportunities for undergraduate, graduate, and continuing medical education. The SP Program manages all aspects of providing professionally trained patients, which includes recruiting, training and scheduling.
The SCSC offers Basic Life Support (BLS) and Advanced Cardiac Life Support (ACLS) training at the center.
The SCSC has an approximately 2,000 square-feet wet lab that provides a unique training environment for all learners. It contains a multitude of partial task trainers, as well as specific equipment such as microscopes for learning.
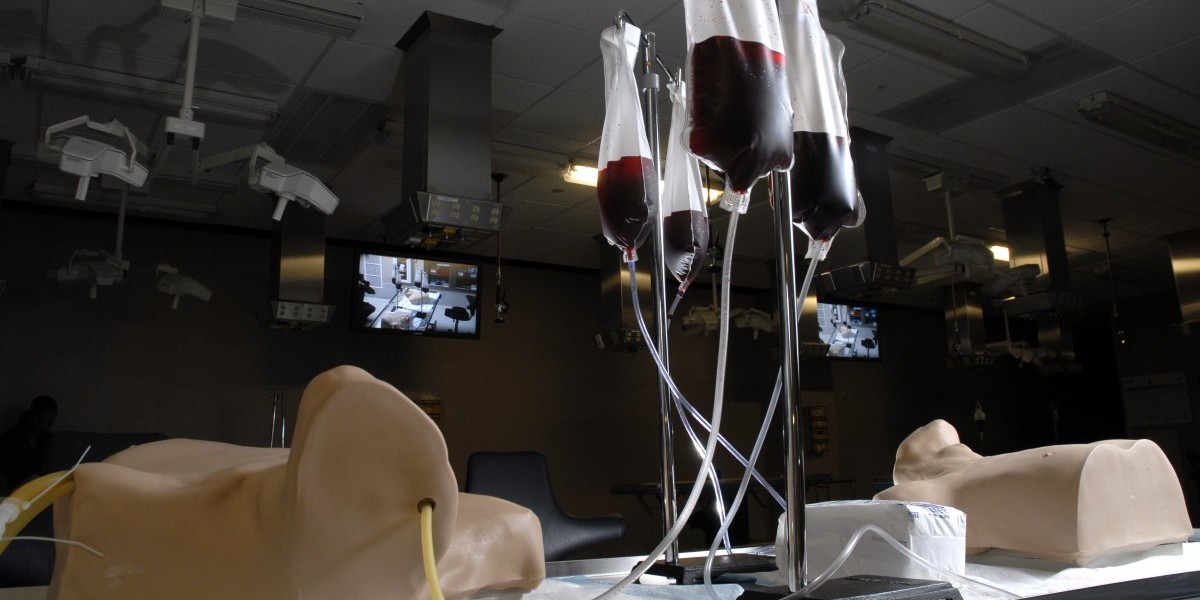
The SCSC has two patient simulation labs that are equipped with high fidelity manikins and standard clinical equipment, monitors, and supplies to simulate operating rooms or emergency rooms. These labs create a realistic environment for trainees to practice and refine important clinical skills from mask ventilation or endotracheal intubation to advanced crisis management.
The SCSC is equipped with the newest telecommunication equipment, including video monitors and two-way communication with a control booth to facilitate teaching and feedback.
The SCSC is located on the basement level of McGovern Medical School. Upon entering McGovern Medical School, take the Yellow elevators to the basement and exit to the left. The main entrance is near the blue wall section.
Surgical Side:
6431 Fannin St.
Suite B.210
Houston TX, 77030
Phone: 713 500-5900
Clinical Side:
6431 Fannin St.
Suite B.120
Houston, TX 77030
Phone: 713 500-5900