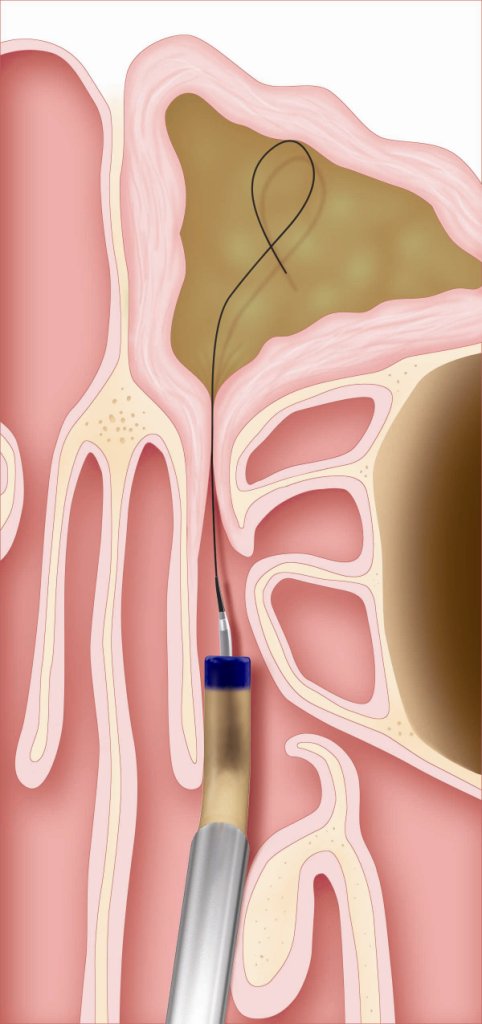
Balloon Sinus Ostial Dilation
What Is Balloon Sinus Ostial Dilation?
Balloon sinus ostial dilation (BSOD) is a procedure during which a slender balloon device is placed across a narrowed sinus ostium and then inflated. The technique is similar to balloon angioplasty, a procedure intended to open narrowed blood vessels that supply blood to the heart.
How Is Balloon Sinus Ostial Dilation An Alternative To Conventional Sinus Surgery?
When balloon sinus ostial dilation (BSOD) was first introduced, some ENT surgeons believed that it was a replacement for conventional endoscopic sinus surgery. Today, most ENT surgeons feel that BSOD is a surgical technique, not a replacement procedure.
Thus, for some patients, BSOD may be part of endoscopic sinus surgery performed using conventional instruments. In other patients, BSOD may be performed as a stand-alone procedure. The decision for using BSOD technology is based upon many factors, including the type and extent of inflammatory disease, patient anatomy and patient preferences.
How is Balloon Sinus Ostial Dilation Performed?
Balloon sinus ostial dilation (BSOD) is a relatively straight forward procedure. Under endoscopic visualization, the sinus balloon device is place into the nasal cavity, and guided to the blocked sinus. Once positioning has been confirmed, the balloon is inflated and then deflated. The device is then removed. The entire procedure must be performed with an emphasis on minimizing trauma to the delicate tissues of the sinus lining.
Two types of sinus balloon devices are available. One uses a flexible guidewire to find the sinus outflow tract. The other uses a malleable rail that is used to find the sinus outflow tract. Of course, there are advantages and disadvantages of each device. Each surgeon will choose the device that he or she feels is most appropriate for the specific surgical target.
At the frontal sinus, BSOD is a four step procedure:
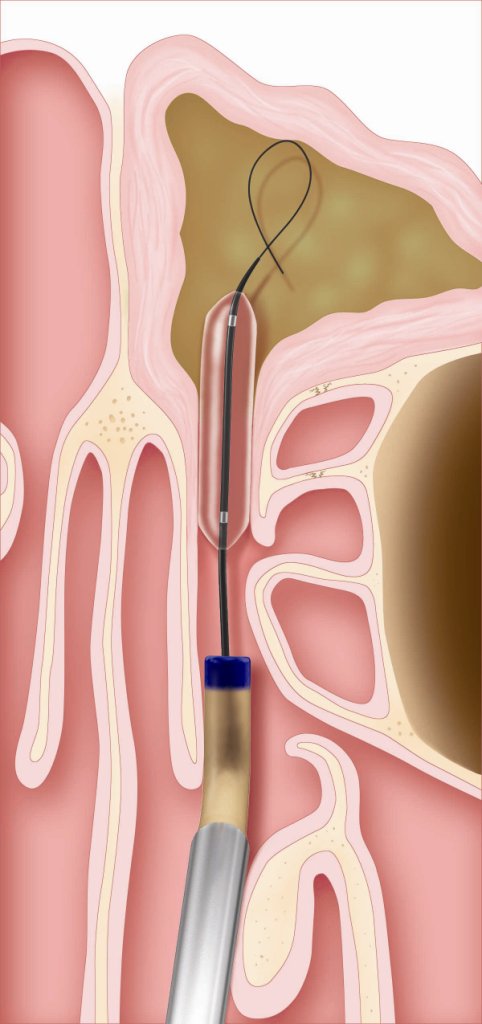
2. The balloon is then introduced over the guidewire and inflated. Then the balloon is removed.
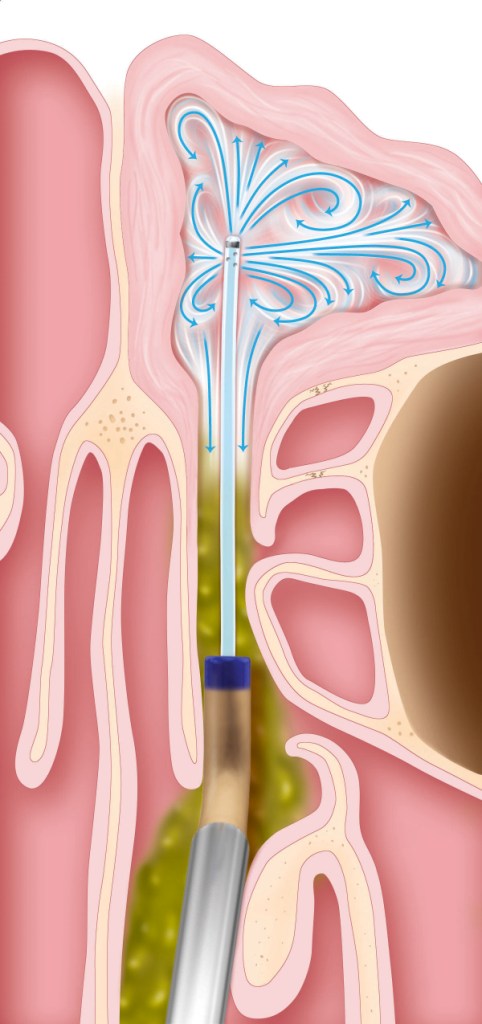
3. The sinus is irrigated. (This is an optional step.)
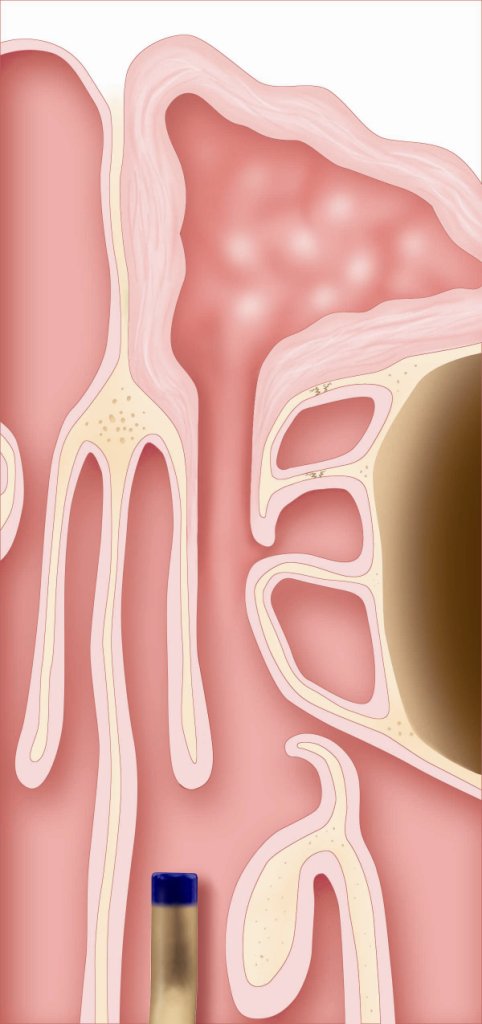
4. The device is removed from the sinus and the opening is inspected via direct visualization.
At the maxillary sinus, BSOD is also a four step procedure:
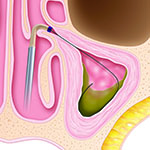
1. A guidewire is placed across the blocked maxillary sinus outflow tract.
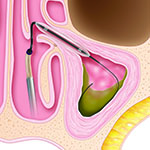
2. The balloon is then introduced over the guidewire and inflated.
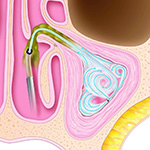
3. The balloon has been removed and then an irrigation catheter is placed over the guide wire. Saline irrigation then flushes debris (mucus and pus) from the maxillary sinus.
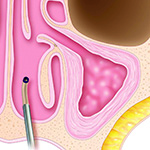
4. The device is removed from the sinus and the opening may be inspected via direct visualization. The maxillary sinus outflow tract has been enlarged. Debris (mucus and pus) is no longer in the maxillary sinus.
Successful BSOD depends upon precise placement of the balloon across the blocked sinus outflow track. Initially, x-rays were used for device placement; however, this is rarely done today. For the frontal and maxillary BSOD, correct placement is confirmed with transillumination; that is, a bright light is passed into the target sinus, and when the light is seen in the forehead (for the frontal sinus) or cheek (for the maxillary sinus) device placement is confirmed.
Recently, microsensors whose position can be determined through a technology known as surgical navigation have been used to confirm device placement.
Where Is Balloon Sinus Ostial Dilation Performed?
Balloon sinus ostial dilation (BSOD) may be performed either in an operating room or in an office setting. The choice of setting is based upon many factors. In general, more extensive or complicated procedures will be performed in an operating room, although recent advances in technique and instrumentation have moved some of these procedures to an office setting.
When the procedure is performed in the operating room, it may be done in a hospital outpatient department or in a dedicated surgical center. Most commonly, the procedure will be done under general anesthesia in these locations. Occasionally, the surgery will be done with intravenous sedation only.
In the office setting, the BSOD may be combined with conventional endoscopic sinus surgery techniques, or BSOD alone may be performed. Regardless, procedures in the office are performed without general anesthesia. Topical medications and local anesthesia provide sufficient comfort for a successful procedure in the office. The main advantage of performing the procedure in the office is a rapid return to normal activity—patients may resume normal activity on the same day in most instances. In addition, scheduling is easier in the office and overall costs are much less.
Who Is A Candidate for Balloon Sinus Ostial Dilation?
The initial treatment for chronic rhinosinusitis is almost always medical. Exceptions to this rule include fungal rhinosinusitis or rhinosinusitis with complications.
When medical treatments fails, then the patient will be a candidate for sinus surgery. The selection of the specific technique is dependent upon many factors, and there are no “hard and fast” rules that guide this process.
The ideal candidate for balloon sinus ostial dilation (BSOD) only procedure has inflammatory disease only in the sinuses that can be addressed with this technique. Thus, patients with sinusitis predominantly in the ethmoid sinuses would not be ideal candidates for a BSOD only procedure. In contrast, patients with sinusitis limited to the frontal, maxillary and/or sphenoid sinuses may be good candidates for BSOD only procedures, especially in the absence of polyps and/or fungal sinusitis.
BSOD may be combined with conventional endoscopic sinus surgery techniques in so-called “hybrid” procedures. This combination is ideally suited for those patients with significant inflammation in the ethmoid sinuses as well as the other sinuses.
The selection of BSOD is a complicated decision. Patients are encouraged to discuss this option with their surgeons so that the right selection is made for each patient.
What Are The Risks Of Balloon Sinus Ostial Dilation?
Balloon sinus ostial dilation (BSOD) is considered a safe procedure. In fact, many surgeons believe that the risks directly related to BSOD are probably less than conventional techniques. (It must be emphasized that conventional endoscopic sinus surgery has also been deemed a “safe” procedure.)
In general, the risks related to BSOD are similar to the risks of conventional endoscopic sinus surgery. Some of these risks are intrinsic to any surgical procedure; there are always concerns about anesthesia reactions, bleeding, scarring and infection. Other risks are related to the location of the sinuses; because the sinuses are located next to the orbits and beneath the brain, the risk of brain or eye injury is always present. Fortunately, the rate of major complications from any sinus procedure are quite low.
Will Balloon Sinus Ostial Dilation Cure My Sinus Problems?
Reported outcomes from balloon sinus ostial dilation (BSOD) are quite good—comparable in many ways to conventional endoscopic sinus surgery. Most patients report dramatic reductions (or even resolution) of their nasal and sinus symptoms after BSOD.
It must be remembered that the main indication for BSD is chronic rhinosinusitis—an inflammatory condition of the nasal lining. Because no surgical procedure can change a patient’s biochemistry, some ongoing medical care will be necessary in selected patients. Thus, any surgical procedure—whether BSOD or conventional endoscopic sinus surgery (or hybrid procedures that incorporate BSOD with standard endoscopic techniques)—should be viewed as one part (albeit an important part) of a comprehensive strategy for reducing and controlling inflammation in the sinuses.