Patient Stories
At the Texas Sinus Institute, our focus is providing successful treatments for all conditions of the nose and sinuses—and an optimal patient experience.

Empty Nose Syndrome: Diagnosis and Management in a 34-Year-Old Patient
The ability to equalize Eustachian tube (ET) pressure is essential for SCUBA divers. As they descend deeper into the water, the outside pressure becomes greater than the air pressure inside the ear. As pressure increases, the eardrums and Eustachian tubes begin to compress.
Read More Empty Nose Syndrome: Diagnosis and Management in a 34-Year-Old Patient

SCUBA Diver Pam Atherton Is Back Underwater
The ability to equalize Eustachian tube (ET) pressure is essential for SCUBA divers. As they descend deeper into the water, the outside pressure becomes greater than the air pressure inside the ear. As pressure increases, the eardrums and Eustachian tubes begin to compress.

Diagnosis, Management, and Prevention of Empty Nose Syndrome
Five years ago, Mablean Warren had surgery for a deviated septum and enlarged turbinates, which were causing nasal obstruction. After her initial satisfaction with the outcome, she began noticing a decrease in her quality of life.
Read More Diagnosis, Management, and Prevention of Empty Nose Syndrome

Transnasal Endoscopic Surgery for a Sphenoid Inverted Nasal Papilloma
The sphenoid sinus is a rare location for an inverted nasal papilloma, a benign but invasive tumor with an associated malignancy rate of about 10%. In 2019, Robert Gum’s family doctor in Georgetown, Texas, identified a large sphenoid tumor when she reviewed his CT scans following a severe concussion he suffered.
Read More Transnasal Endoscopic Surgery for a Sphenoid Inverted Nasal Papilloma

Repair of a Left Ethmoid Cerebrospinal Fluid Leak
For months, Janie Lee’s nose wouldn’t stop running. Clear fluid ran from her left nostril during the day and down her throat at night. A nurse at Woodland Heights Medical Center in Lufkin, Texas, Lee stuffed tissue in her nostrils and put a mask on when she was called to see a patient.
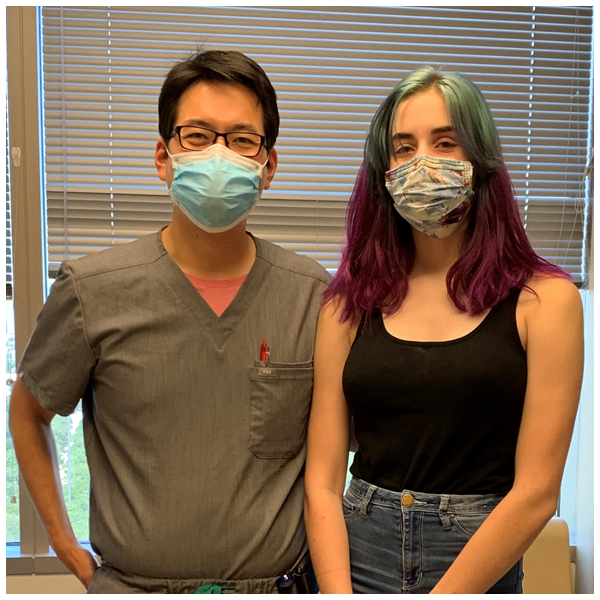
Endoscopic Surgery for a Rare Presentation of Sinonasal Osteoma
When an MRI revealed a mass in Phoebe’s left sinus extending behind the eye, her pediatrician referred her to William Yao, MD, a fellowship-trained rhinologist and assistant professor in the Department of Otorhinolaryngology-Head and Neck Surgery at McGovern Medical School at UTHealth.
Read More Endoscopic Surgery for a Rare Presentation of Sinonasal Osteoma

Minimally Invasive In-Office Treatment for Nasal Polyps
Rick Jackson was failing maximal medical treatment and well on his way to a third trip to the OR for nasal polyposis, when his rhinologist Martin J. Citardi, MD, suggested that he try SINUVA®.
Read More Minimally Invasive In-Office Treatment for Nasal Polyps

The Perfect Candidate for Dupilumab
Curtis Griffin was on the verge of a sixth surgery for nasal polyposis when his rhinologist suggested that he try dupilumab, a monoclonal antibody approved by the U.S. Food and Drug Administration to treat asthma, atopic dermatitis, and chronic rhinosinusitis with nasal polyps (CRSwNP).

The Perfect Candidate for Dupilumab
Scott Nickell was among the millions of people who suffer from difficulty breathing through the nose. Until recently his only options were medications or breathing strips that offer temporary relief, or invasive surgeries that involve a period of recovery.
Read More Minimally Invasive Nasal Remodeling Helps a Patient Breathe More Easily

Treating Nasal Polyps due to AERD with Revision Sinus Surgery and Aspirin Desensitization
For two decades Cobb saw various ENTs and tried a variety of oral and nasal medications for chronic rhinosinusitis, without sustained relief. In the process, he was diagnosed with Samter’s Triad, a chronic condition defined by asthma, sinus inflammation with difficult-to-treat nasal and sinus polyps, and aspirin sensitivity.
Read More Treating Nasal Polyps due to AERD with Revision Sinus Surgery and Aspirin Desensitization

Minimally Invasive Nasal Remodeling Procedure Allows Patients with Obstruction to Breathe More Easily
After receiving information about the availability of the VivAer® nasal airway remodeling procedure, Smith scheduled an appointment with William C. Yao, MD, an assistant professor and rhinologist in the Department of Otorhinolaryngology-Head and Neck Surgery at McGovern Medical School at UTHealth

Nasopharyngeal Carcinoma (NPC): Treating a Rare, Aggressive Tumor with Skill and Compassion
Spike Sturdivant found the medical and moral support he needed in otorhinolaryngologist Amber Luong, MD, PhD, and radiation oncologist Angel Blanco, MD, after being diagnosed with nasopharyngeal carcinoma in early 2018.

New Nonsurgical Treatments for Nasal Polyps Help Patients Breathe Again
“When my condition worsened, I did my homework on alternatives to surgery for polyps,” Toufeeq says. “My first endoscopic sinus surgery was not an ordeal, and I was home in two hours flat. Still, surgery is surgery and why go through it if you can find something else that works?”
Read More New Nonsurgical Treatments for Nasal Polyps Help Patients Breathe Again

Cherry-on-Top Surgery Helps Larry Simmons Smell and Taste Again
“I didn’t even notice it,” says Simmons, 72. “I couldn’t breathe through my nose, so I just started breathing through my mouth. My first medication was a nasal spray, but it didn’t help.”
Read More Cherry-on-Top Surgery Helps Larry Simmons Smell and Taste Again

Intranasal Cryoablation: A Breakthrough for Postnasal Drip and Chronic Rhinitis
“For a year my voice sounded like I had gravel in my throat,” says Olin, 59. “My sinuses drained so much and so fast that I would literally choke. I sneezed constantly, and my life was totally miserable. When Dr. Stanley told me about ClariFix, I said, yes, I’ll try anything to get off steroids and antibiotics.”
Read More Intranasal Cryoablation: A Breakthrough for Postnasal Drip and Chronic Rhinitis
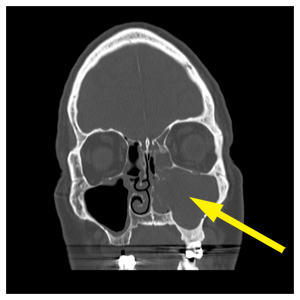
Minimally Invasive Surgery Provides Quick Relief of Sinusitis Caused by a Dental Infection
An accurate diagnosis and effective treatment dramatically improved the life of 75-year-old Ed Dickerson, whose off-and-on history of nasal congestion goes back to his childhood.
Read More Minimally Invasive Surgery Provides Quick Relief of Sinusitis Caused by a Dental Infection
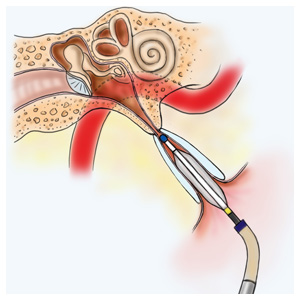
Balloon Eustachian Tuboplasty for Chronic Eustachian Tube Dysfunction
Two weeks after having balloon eustachian tuboplasty, Robin Goebel was on a flight to South America, where she hiked at high altitudes, visiting Machu Picchu at 7,970 feet and Cusco at 11,152 feet, and took 13 different flights to places ranging from Ecuador to the Galapagos Islands.
Read More Balloon Eustachian Tuboplasty for Chronic Eustachian Tube Dysfunction
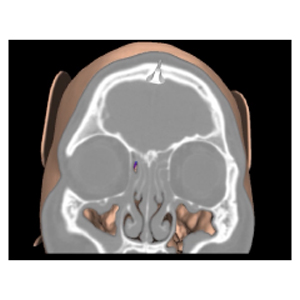
Herbert Ross: Among the First in the U. S. to Benefit from a New Surgical Navigation System
Ross had undergone an earlier surgery for removal of nasal polyps in 2007. “They came back with a vengeance,” he says. “For the last two or three years, I could hardly breathe at all out of my right nostril, especially during the spring, and nasal sprays didn’t help. ”
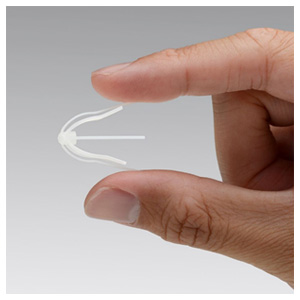
Carrie Owen Benefits from a New Minimally Invasive In-office Treatment for Nasal Polyposis
Owen, 41, had problems with asthma, allergies and nasal polyps for years and, after losing the ability to smell and taste, was told by her ENT in College Station that she needed surgery. She underwent a nasal polypectomy in May, 2017.
Read More Carrie Owen Benefits from a New Minimally Invasive In-office Treatment for Nasal Polyposis
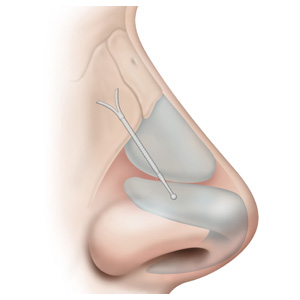
Breathing Better After Surgery and a Novel Implant
Krohn, 27, first met her surgeon William C. Yao, MD, after experiencing ringing in her ears. During the course of her office evaluation, he also diagnosed her with a significant deviated nasal septum and inferior turbinate hypertrophy.
Read More Breathing Better After Surgery and a Novel Implant
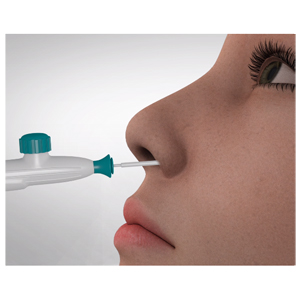
Breakthrough Treatment for Chronic Rhinitis & Postnasal Drip
As he grew older, 42-year-old Jon Balter developed severe chronic rhinitis and sought help from allergists and ENTs for nearly a decade. After trying allergy shots and a variety of medications without success, he was referred by his allergist to Martin J. Citardi, MD, who used a breakthrough cooling technology to treat the disorder successfully.
Read More Breakthrough Treatment for Chronic Rhinitis & Postnasal Drip

Norman Theeck Makes a Comeback from Invasive Fungal Rhinosinusitis
In December 2012, Theeck went to his local ENT in Beaumont, Texas, complaining of bad sinus headaches. “Because I have heart disease, he didn’t want to put me under anesthesia, so he asked me how tough I am. ‘Pretty tough,’ I said.
Read More Norman Theeck Makes a Comeback from Invasive Fungal Rhinosinusitis

Revision Sinus Surgery Sets the Stage for a Successful Outcome
Revision endoscopic sinus surgery presents challenges not often seen in primary surgeries. Rhinologists at Memorial Hermann-Texas Medical Center and McGovern Medical School at UTHealth routinely treat refractory conditions in patients from Houston as well as the entire state of Texas.
Read More Revision Sinus Surgery Sets the Stage for a Successful Outcome

Dissolvable Steroid Implant May Improve Sinus Surgery Outcomes
“We found that the implants were associated with improved endoscopic surgical outcomes for sinusitis,” said Amber Luong, M.D., Ph.D., the study’s lead author and the director of research in the Department of Otorhinolaryngology.
Read More Dissolvable Steroid Implant May Improve Sinus Surgery Outcomes
Otorhinolaryngology and Neurosurgery Team Up to Maximize the Outcome for a Patient with Pituitary Tumor
After an unexplained “brain glitch” led to the discovery of a large pituitary tumor, retired corrosion engineer Niell Strickland joined the ranks of patients who have benefited from the teamwork of rhinologist William Yao, MD , and neurosurgeon Spiros Blackburn, MD.
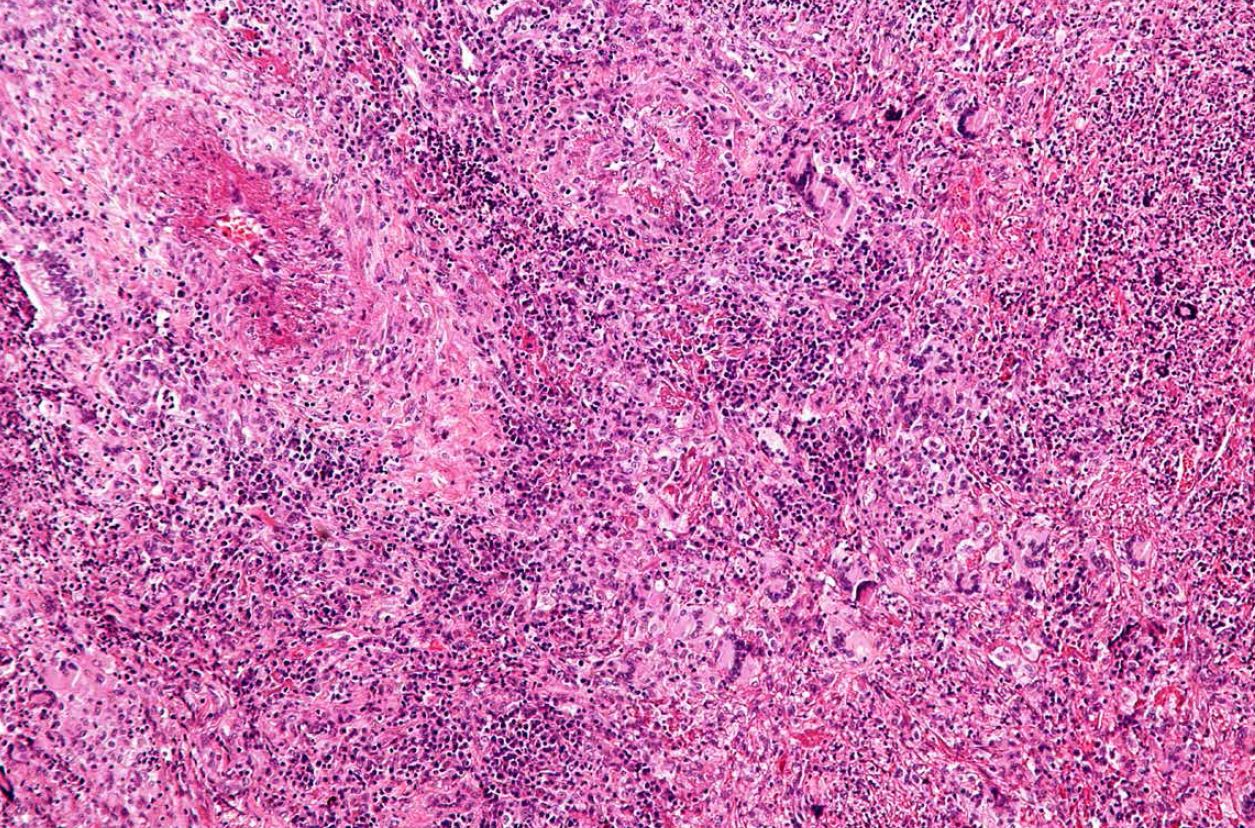
Granulomatosis with Polyangiitis: A Patient Benefits from Multidisciplinary Care
“I was 57 and had never been sick a day in my life when I suddenly developed a severe sinus infection,” says Giles, who lives in Spring, Texas. “My wife and I were scheduled to go to Kentucky to visit her parents, so I went to a family doctor on the north side of Houston who prescribed medication to treat the symptoms. I still felt bad, and when we landed in Knoxville, I thought my eardrums had burst.”
Read More Granulomatosis with Polyangiitis: A Patient Benefits from Multidisciplinary Care

Drug-Eluting Stent for Chronic Rhinosinusitis
After suffering for years from severe allergic fungal rhinosinusitis, Wynard De’kavon Crawford found relief through a minimally invasive office procedure: the placement of a tiny PROPEL® mini dissolvable implant into each of his ethmoid sinuses.

Breath of Fresh Air
Butcher, her husband Larry and their three daughters moved from California to Corpus Christi in 1979, when Larry took a job in the oilfields. Aside from the occasional head cold, Butcher, 68, who works at a Ford dealership, had always enjoyed good health—and playing sports.

Skull Base Cancer
Toward the end of 2010 and well into 2011, 32-year-old Kurtis White had a persistent runny nose that he assumed was caused by allergies. After trying various over-the-counter medications for nearly six months—without relief—he made an appointment with his primary care physician.

Morphoproteomics
s she was preparing to leave for a semester abroad in Europe, 20-year-old Baylor University student Bridgette Marshall heard news she never expected to hear. Her otorhinolaryngologist Martin J. Citardi, MD, FACS, told her she had a very rare and advanced form of cancer.

Setting a Good Course
Richard Petty doesn’t normally write laudatory letters about his physicians, but after treatment for chronic rhinosinusitis (CRS), he sat down and penned one to Giuseppe Colasurdo, MD, president of The University of Texas Health Science Center at Houston and then dean of the UTHealth John P. and Kathrine G. McGovern Medical School.
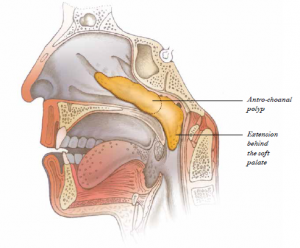
Proteus Syndrome
By the time 39-year-old Ricky Watson saw Amber Luong, MD, PhD, FACS, he could no longer swallow, eat or talk. His only avenue of communication with his family was writing on a notepad or texting via cell phone. Diagnosed at the age of 10 with Proteus syndrome, an extremely rare condition marked by overgrowth of bones, skin and other tissues, Watson had undergone numerous surgeries at institutions in East and West Texas in failed attempts to correct conditions caused by the syndrome.

